Two articles from reputable Diabetes Medical Journals in 2000 and in 1998, suggest that diabetics should not drive if their blood glucose is below 100mg/dl (6.7mmol/L)
Diabetes, hypoglycaemia ( hypoglycemia , insulin shock, insulin reaction ) and driving capacityOriginal article: Thirty-seven
adults with Type 1 diabetes drove a
simulator during continuous euglycaemia and
progressive hypoglycaemia ( hypoglycemia ,
insulin shock, insulin reaction ). During
testing, driving performance, EEG and
corrective behaviours (drinking a soda or
discontinuing driving) were continually
monitored, and blood glucose, symptom
perception and judgement concerning
impairment were assessed every 5 min. Mean
± SD euglycaemia performance was used to
quantify z-scores for performance in three
hypoglycaemic ranges: 4.0–3.4, 3.3–2.8
and <2.8 mmol/l. During
all three hypoglycaemic blood glucose
ranges, driving was significantly impaired
and subjects were aware of their impaired
driving. However, corrective actions did not
occur until blood glucose was <2.8
mmol/l. Driving impairment was related to
increased neurogenic symptoms and increased
theta-wave activity. Awareness of impaired
driving was associated with neuroglycopenic
symptoms, increased beta-wave activity, and
awareness of hypoglycaemia ( hypoglycemia ,
insulin shock, insulin reaction ). High
beta- and low theta-wave activity and
awareness of both hypoglycaemia (
hypoglycemia , insulin shock, insulin
reaction ) and the need to treat low blood
glucose influenced corrective behaviour. The
authors conclude that driving performance is
significantly disrupted at relatively mild
hypoglycaemia ( hypoglycemia , insulin
shock, insulin reaction ), yet subjects
hesitated to take corrective action. The
longer treatment is delayed, the greater the
neuroglycopenia (increased theta-wave
activity), which precludes corrective
behaviours. Patients should self-treat while
driving as soon as low blood glucose and/or
impaired driving is suspected and should not
begin driving when their blood glucose is in
the 5.0–4.0 mmol/l range without
prophylactic treatment. Comment It is
now well established that people with
diabetes as a group do not have higher
accident rates than their non-diabetic
counterparts [1–6]; two studies even
suggest a decreased risk among people with
diabetes [7, 8]. This might be explained by
the fact that people with diabetes as a
group drive more carefully (e.g. lower
alcohol consumption, more frequent stops
during long distance drives, better respect
for general driving regulations). Moreover,
whereas alcohol is the most important human
factor in road traffic accidents,
hypoglycaemia ( hypoglycemia , insulin
shock, insulin reaction ) is very rarely
implicated [9]. These favourable
observations mean that insulin-treated
people in most countries of the world face
no additional restrictions to their ability
to hold a driving licence. However
amongst those with insulin-treated diabetes,
some may indeed be at high risk of road
traffic accidents, i.e. those with impaired
hypoglycaemia ( hypoglycemia , insulin
shock, insulin reaction ) awareness, a
phenomenon that may be present in up to 25%
of Type 1 diabetics [10, 11]. Clearly,
access to a driving licence (for both
professional and private purposes) should be
strictly regulated in those with
hypoglycaemia ( hypoglycemia , insulin
shock, insulin reaction ) unawareness, and
the technique for restoring hypoglycaemia (
hypoglycemia , insulin shock, insulin
reaction ) awareness by avoiding
hypoglycaemic episodes for several weeks
should be widely used [12, 13]. This
study by Cox et al. once more underlines the
importance of the problem of reduced
hypoglycaemia ( hypoglycemia , insulin
shock, insulin reaction ) awareness: 15% of
the 37 subjects tested detected
hypoglycaemia ( hypoglycemia , insulin
shock, insulin reaction ) when their blood
glucose value was between 4.0 and 3.4
mmol/l; 33% when their blood glucose value
was between 3.3 and 2.8 mmol/l; and 79% when
their blood glucose fell below 2.8 mmol/l
(Table I).
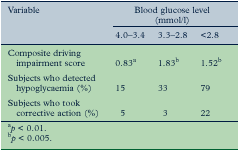
Table I: Driving performance at three levels of hypoglycaemia ( hypoglycemia , insulin shock, insulin reaction ). Above
all, it specifically emphasizes the fact
that even when subjects recognized their
hypoglycaemic state, only 5% took corrective
action at blood glucose 4.0–3.4 mmol/l, 3%
at blood glucose 3.3–2.8%, and 22% at
blood glucose <2.8 mmol/l (Table I),
indicating that more than 70% of the tested
subjects, under experimental driving
conditions, did not take corrective action
for their hypoglycaemia ( hypoglycemia ,
insulin shock, insulin reaction ) even at a
blood glucose level below 2.8 mmol/l.
Moreover their driving performance score was
significantly reduced during hypoglycaemia (
hypoglycemia , insulin shock, insulin
reaction ) (p < 0.01 for blood glucose
4.0–3.4 mmol/l and p < 0.005 for blood
glucose 3.3–2.8 and <2.8 mmol/l) (Table
I). This
study demonstrates that hypoglycaemia (
hypoglycemia , insulin shock, insulin
reaction ) is a significant factor in
impaired driving and that patients are
generally aware of when their driving
performance is deteriorating. However, the
data also indicate that patients are
unlikely to treat their low blood glucose
while driving. In large part, this appears
to be due to waiting too long before taking
corrective action. The results therefore
suggest that patients should be encouraged
to treat themselves immediately, whenever
they think their blood glucose is low or
their driving ability is impaired, and not
wait until they become too neuroglycopenic
or their driving ability too impaired. As
stated by Marrero and Edelman in their
editorial [14]: ‘It is obviously important
that we teach strategies for avoiding
hypoglycaemia ( hypoglycemia , insulin
shock, insulin reaction ) that are specific
to driving. Blood glucose testing before
driving needs to be stressed and minimum
glucose values for safely operating a motor
vehicle need to be established.’ Diabetes educators should impress on their patients the importance of:
|
|
ADA CONFERENCE: Mild Hypoglycemia Impairs Driving In Type I Diabetics CHICAGO, IL -- June 16, 1998 --
For people with Type I diabetes, episodes of
even mild hypoglycemia can make driving
dangerous, according to researchers at the
University of Virginia Health Sciences
Center. The finding was reported today
at the annual meeting of the American
Diabetes Association in Chicago. "Based on the results of
this study, we are recommending that people
with diabetes should never get behind the
wheel of a car if their blood glucose level
is 80 mg/dl or less," said Daniel Cox,
professor of psychiatric medicine at U.Va.
and the study's lead investigator. "If
they are driving and suspect that their
blood glucose is getting low, they should
pull over and treat it immediately." Prior to the U.Va. study,
doctors thought that a blood glucose level
of less than 60mg/dl could result in
impaired driving capability. Hypoglycemia
starves the brain of glucose energy, which
is essential for proper brain function. Lack
of glucose energy to the brain can cause
symptoms ranging from headache, mild
confusion and abnormal behaviour to loss of
consciousness, seizure and coma. In the U.Va. study, 37 adults
with Type I diabetes and a history of severe
hypoglycemia were tested using a
sophisticated driving simulator and a
gradual induction of hypoglycemia. During
the two, 30-minute testing sessions, the
subjects' driving performance,
electroencephalogram (EEG) and
self-treatment of low blood glucose (BG)
were continually monitored. At the same
time, BG level, symptom perception and
judgement concerning driving impairment and
the need to self treat were assessed every
five minutes. To objectively assess driving
in a controlled environment, the Atari
Research Driving Simulator was utilised. The
simulator has three, 25-inch computer
screens that wrap around the driver,
providing a 160- degree visual field, along
with a programmed rear view mirror depicting
rear traffic. The driving environment was
realistic, incorporating a typical-sized
steering wheel, gas and brake pedals, seat
and seat belt, Cox said. Driving performance feedback
was provided to the subject visually through
the three screens that updated at a rate of
60 times per second; aurally through
quadraphonic speakers delivering engine,
tire and road noises; and kinesthetically
through the steering wheel and pedal
pressure. Patients were kept blind to the BG
manipulations and actual BG levels. Results of the study show that
driving was significantly impaired during
all three hypoglycemic BG ranges tested --
72 to 61, 60 to 50 and less than 50 mg/dl.
In addition, subjects were aware of both the
need to treat their low BG and their
impaired driving. However, actual treatment
of low BG did not occur until BG was less
than 50 mg/dl. "Although other studies
show that individuals with diabetes have no
more driving accidents than the general
population, when they do, it is often due to
hypoglycemia," Cox said.
"Prevention of hypoglycemia-related
accidents relies on both a driver's ability
to recognise that BG is low and then to take
corrective actions of consuming
carbohydrates and/or pulling off the road. “Our study showed that
even when the subjects suspected that their
blood glucose was low, they waited too long
to treat it, with potentially dangerous
consequences." Editorial notes: Much of what is being said here is simply not true. The Frequency and Incidence of Diabetic Automobile accidents has been rising dramatically since 1983. The Facts reveal that 60-70% or more of diabetics suffer unnoticed hypoglycemia well below 60 mg/dl (4.0 mmol/L) on the "new" synthetic insulins when they use the MiniMed CGM (Continuous Glucose Monitor). This shows the propagandistic lies of blaming the patient for waiting too long. If you do not have hypoglycemia symptoms, you can't be waiting, you are too busy dying, maiming yourself or doing one or the other to innocent bystanders! We have been trying to warn the diabetes community of this problem since February of 1989. Don't even turn you car on if your BG is below 100 mg/dl or 5.5 mmol/L!! That is the experts, NOT me saying this. PLEASE DON'T DRIVE WITH A BG UNDER 100 mg/dl (6.7 mmol/L). |