
CARDIAC RATE AS PREDICTOR OF THYROID FUNCTION
IN PATIENTS WITH ENLARGED THYROID GLAND
JANIX M. DE GUZMAN, M.D.
CATHERINE CO, M.D.
EDGARDO S. PENSERGA, M.D., FPSGS, FPCS
REYNALDO O. JOSON, MD, MHA, MHPED, MS SURG
Abstract:
OBJECTIVE: To validate the diagnostic value of cardiac rate in assessing the thyroid function of a patient with thyroid enlargement. METHODS: Retrospective analysis of cases seen at the Out-patient Section (OPS), Department of Surgery of a tertiary government hospital for January 2002 to December 2004 and OPS, Department of Surgery of a tertiary private hospital from February to September 2004 in Metro Manila. RESULTS: 110 patients with enlarged thyroid gland were included in this study. Cardiac rate was compared to result of (thyroid stimulating hormone) TSH assay and measures of efficacy determined. Sensitivity and specificity changed for different set of patients. For all patient with thyroid enlargement overall sensitivity and specificity were 92% and 95%; for diffuse, 95% and 67%; for nodular, 80% and 97%, respectively. Positive predictive value (PPV), negative predictive value (NPV), and prevalence were also determined. Overall, PPV=85%, NPV=98%, prevalence=23%. For diffuse, PPV=90%, NPV=80%, prevalence=77%. For nodular, PPV=67%, NPV 99%, prevalence=6%. CONCLUSION: Overall, cardiac rate has a high sensitivity and specificity as well as PPV and NPV to patients with enlarged thyroid gland. It became more sensitive and PPV increased when used to patients with diffusely enlarged thyroid gland and more specific as well as higher NPV to nodularly enlarged thyroid gland.
Keywords: cardiac rate, thyroid stimulating hormone
Introduction:
The last decade of 20th century marked the development of supersensitive second- and third-generation thyroid stimulating hormone (TSH) assays that made TSH measurement as the single most useful test of thyroid function. These second- and third-generation TSH assays can distinguish euthyroid patients from hyperthyroid patients in the general population (1). However, instead of using this new diagnostic modality judiciously as support for accurate diagnosis it became an essential or routine for physicians to request these assays resulting in disproportionately large expenditures on laboratory resources (2). Hence, we failed to take advantage of the cost effectiveness of these assays. We must remember that clinical findings can yield accurate and efficient answers to questions pertinent to the diagnosis and treatment of thyroid patients. The optimal use of thyroid function test is patient-specific and depends on the patient’s specific thyroid disease.
In our institution, since 2002, the Department of Surgery has adopted a selective pre-operative screening. This was piloted on patients with operable thyroid nodules eliminating unnecessary laboratory examinations, endocrine, cardiac and pulmonary clearances. The Department utilizes clinical evaluation: good history taking and thorough physical examination. Through these the clinician then decides if the patient needs additional paraclinical diagnostic examination (3).
In a patient with thyroid enlargement, diffuse or nodular, determined by physical examination through palpation, we only utilizes full minute cardiac rate to assess thyroid function. If more than 90 beats per minute (bpm) was noted in a rested patient with thyroid enlargement, TSH and Free thyroxine (FT4) assays will then be requested. If less than or equal to 90 bpm was noted especially on nodular gland, solitary or multi-nodular, patient will be scheduled for operation if indicated without determining thyroid function tests provided suspicion on malignancy is eliminated as well as co-morbid conditions were fully addressed, if any (Figure 1). This paper will not discuss treatment nor will go into the details of malignant investigation.
Worldwide, in the general population, thyroid nodules are the commonest disorder presenting to the endocrine surgeon (4,5). They occur in 4 to 7 percent of the population (10 to 18 million persons) (6). In the Philippines, majority of Filipino patients with a thyroid problem also present with a nodular goiter in which colloid adenomatous goiter is the most common, 80 per cent of cases (7). The majority of these patients with thyroid nodules are euthyroid because goitrous changes in the thyroid gland or the development of thyroid nodules often do not alter thyroid function (8,9). The integrity of thyroid function can be assessed in two ways, clinical and/or biochemical. However, the complexity and subjectiveness of Wayne’s clinical index (10) and the frequent unavailability of biochemical testing in our institution made the Department of Surgery to adopt the most objective clinical finding of cardiac rate alone as predictor for thyroid function in patients with enlarged thyroid gland since 2002. For this reason it is the aim of this study to validate the diagnostic value of cardiac rate in assessing the thyroid function of a patient with thyroid enlargement.
Methods:
Retrospective reviews of available cases since January 2002 to December 2004 at the out-patient section of the department of surgery at a tertiary government hospital in Metro Manila, and patients seen and screened for the in-house thyroid mission of the department of surgery at a tertiary private hospital in Metro Manila from February to September 2004 were done. All patients with enlarged thyroid gland and with thyroid function tests at least TSH assays were included. The enlarged thyroid gland was determined by palpation and labeled as either diffuse, solitary nodule, or multi-nodular. To be considered diffuse, a goiter must cross the midline of the neck and should be consistent in character, or any inconsistency should be generalized (11). A thyroid nodule is a swelling that develops in the thyroid gland. It can be due to growth of thyroid cells or a collection of fluid known as a cyst (12). The cardiac rates or pulse rates for each patient were gathered. Other data included were the age and sex of the patients.
Excluded were patients with thyroid nodules not detected by physical examination through palpation and only determined by imaging modalities and those patients with overt and subclinical hypothyroidism. Also excluded were patients who had received prior treatments for their current thyroid problem and patients receiving medications that directly or indirectly affects their cardiac rate for any other indications.
The demographic profile of the study population was determined. The cardiac rates were validated against the results of TSH assays which were referred to as reference or gold standards using two by two table. Patients with less than or equal to 90 bpm were labeled as in euthyroid state and those with more than 90 bpm were labeled as in hyperthyroid state (13). Compared to TSH assays, patients with decreased TSH assays were labeled as having true hyperthyroidism and patients with normal TSH assays as healthy or as having true euthyroid state. The sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV), and prevalence were determined.
Results:
A total of 110 patients were included in this study (Table 1). Majority (91%) were females (Figure 2). The ages ranged from 14 to 72 years. Most of the patients were on their third decade of life with a mean age of 36.8 years (Figure 3).
The characters of the thyroid enlargement were categorized into either diffuse or nodular. If determined to be nodular it was further classified into solitary or multi-nodular. Most of the subjects (76%) demonstrated thyroid nodules, 61 of which were solitary and 23 were multi-nodular. The rest (24%) of the study populations were determined to have diffuse thyroid enlargement (Figure 4).
There were 83 patients determined to have cardiac rate less than or equal to 90 bpm while the other 27 patients demonstrated more than 90 bpm on their cardiac rate (Table 2).
The overall sensitivity and specificity of the cardiac rate in predicting hyperthyroidism or euthyroidism when applied to all patients with thyroid enlargement were 92 per cent and 95 per cent, respectively. In the general set of population with thyroid enlargement the prevalence of them experiencing hyperthyroidism was 23 per cent. The PPV and NPV were 85 per cent and 98 per cent, respectively (Table 3).
When considered separately, those with diffused enlargement of thyroid gland using cardiac rate alone as predictor of hyperthyroidism has a sensitivity of 95 per cent but has reduced specificity of 67 per cent. The PPV and NPV were determined to be 90 per cent and 80 per cent, respectively. It was also noted that diffuse thyroid enlargement has a high chance of increased cardiac rate with 77 per cent of them having more than 90bpm cardiac rate most of the time (Table 4).
For nodular enlargement of the thyroid gland, when cardiac rate was used as predictor to assess thyroid function it gave a sensitivity of 80 per cent and specificity of 97 per cent. The PPV was 67 per cent and NPV was 99 per cent in a 6 per cent pre-test probability or prevalence (Table 5).
Discussion:
Cardiac rate though considered non-specific clinical screening tool for thyroid function status of the general population exhibited highly reliable sensitivity and specificity results when applied to patients with thyroid enlargement. It was determined that cardiac rate is more sensitive if used on a subset of population with diffuse enlargement of the thyroid gland and more specific to patients with nodular enlargement of the thyroid gland. These results fortified and validated our stand on the judicious use of TSH assays on patients with enlarged thyroid gland especially those with nodular enlargement and be limited only to patients exhibiting higher cardiac rate of 90 bpm. Our department continued to use this guideline and had been in effect since 2002. The results of this strategy proved worthy as we have limited some financial burden on a lot of patients, decreased out-patient department (OPD) visits, and markedly reduced waiting time or delay for treatment. Based on our annual reports from 2002 to 2004, we have operated on a significant number of patients (272 thyroidectomies) without a single morbidity recorded which was associated with hyperthyroidism or thyrotoxicosis while we continue to implement a selective pre-operative screening approach to date.
To be cautious on the other side, it is noteworthy to point out that specificity of cardiac rate was low (67%) in patients with diffuse enlargement of the thyroid gland. Also, the prevalence of hyperthyroidism was determined to be high (77%) on patients with diffuse enlargement of the thyroid gland and NPV of cardiac rate was only 80 per cent. Hence, it would also be prudent to request TSH assay and free thyroxine (FT4) on this subset of patients as this would also identify patients with subclinical hyperthyroidism (14,15). Fortunately, diffuse enlargement of the thyroid gland share only 24 per cent of the total patient population with enlarged thyroid glands.
The limitation of this study was detecting patients with subclinical hypothyroidism as signs and symptoms of overt hypothyroidism could be detected clinically. Prevalence of subclinical hypothyroidism increases with age starting at 50 and has female preponderance. Among women 50 years of age and older, the prevalence of subclinical hypothyroidism was 5 to 10 per cent (16). Applying it to our set of population in which 14 per cent belongs to women 50 years and older, we could have missed 0.7 to 1.4 per cent of the total population. However, it would be nice to know that most patients found by screening to have subclinical hypothyroidism have at least one symptom that could be related to this diagnosis. Therefore, for high risk individual be particular to these following symptoms, which include muscle cramps, dry skin, intolerance to cold, constipation, poor energy levels, fatigue, and mental slowness (16).
Overall, the data had shown that cardiac rate alone could give highly reliable information on the thyroid function status of patients with enlarged thyroid gland. That this information could facilitate our decision making regarding judicious requesting of subsequent thyroid function assays.
References:
Table 1. Age and Sex Distribution of the study population.
|
Age |
Male |
Female |
Total |
|
< 20 |
0 |
3 |
3 |
|
21 – 30 |
3 |
32 |
35 |
|
31 – 40 |
1 |
35 |
36 |
|
41 – 50 |
3 |
15 |
18 |
|
51 – 60 |
3 |
13 |
16 |
|
61 – 70 |
0 |
1 |
1 |
|
> 70 |
0 |
1 |
1 |
|
|
10 |
100 |
110 |
Table 2. Distribution of study population according to cardiac rate.
|
Cardiac Rate |
Number |
|
< 60 |
3 |
|
61 – 70 |
9 |
|
71 – 80 |
39 |
|
81 – 90 |
32 |
|
91 – 100 |
15 |
|
101 – 110 |
7 |
|
111 – 120 |
3 |
|
> 120 |
2 |
|
Total |
110 |
Table 3. Overall distribution of study population according to cardiac rate and TSH result.
|
Cardiac Rate |
TSH decreased |
TSH Normal |
Total |
|
|
> 90 bpm |
23 |
4 |
27 |
PPV = 85% |
|
< 90 bpm |
2 |
81 |
83 |
NPV = 98% |
|
Total |
25 |
85 |
110 |
|
|
|
Sensitivity = 92% |
Specificity = 95% |
Pre-Test Probability = Prevalence = 23% |
|
Table 4. Distribution according to cardiac rate and thyroid function tests on diffusely enlarged thyroid gland.
|
Cardiac Rate |
TSH decreased |
TSH Normal |
Total |
|
|
> 90 bpm |
19 |
2 |
21 |
PPV = 90% |
|
< 90 bpm |
1 |
4 |
5 |
NPV = 80% |
|
Total |
20 |
6 |
26 |
|
|
|
Sensitivity = 95% |
Specificity = 67% |
Pre-Test Probability = Prevalence = 77% |
|
Table 5. Distribution according to cardiac rate and thyroid function tests on nodularly enlarged thyroid gland.
|
Cardiac Rate |
TSH decreased |
TSH Normal |
Total |
|
|
> 90 bpm |
4 |
2 |
6 |
PPV = 67% |
|
< 90 bpm |
1 |
77 |
78 |
NPV = 99% |
|
Total |
5 |
79 |
84 |
|
|
|
Sensitivity = 80% |
Specificity = 97% |
Pre-Test Probability = Prevalence = 6% |
|
Figure 1. General Guidelines for patients with Thyroid Enlargement.

Figure 2. Sex Distribution.

Figure 3. Age and Sex Distribution.
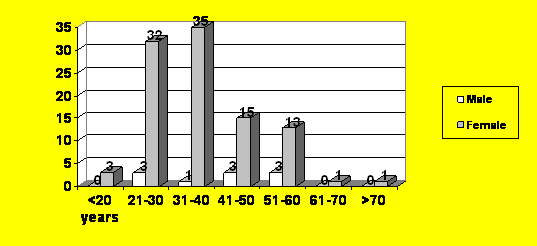
Figure 4. Distribution according to character of thyroid enlargement.
