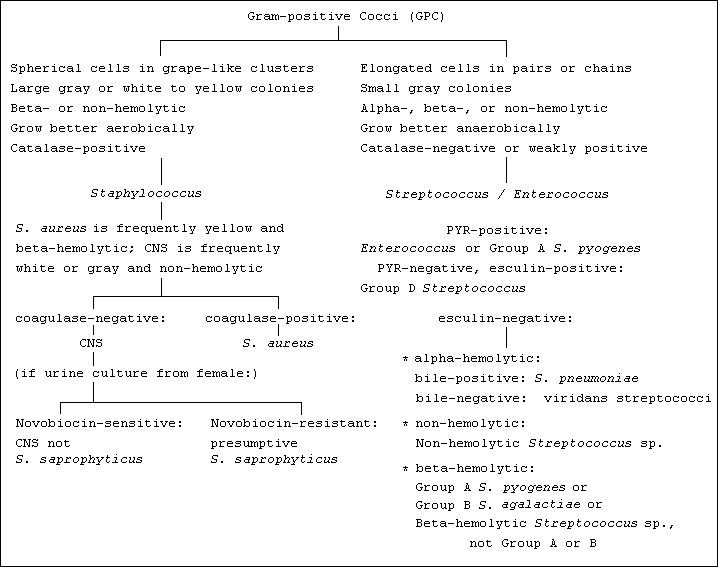
Gram-positive cocci (GPC) are seen on a Gram stain. If they occur primarily as mostly spherical cells arranged in grape-like clusters, then they can be reported as resembling staphylococci. On the other hand, if they occur primarily as somewhat elongated cells arranged in pairs or chains, then they can be reported as resembling streptococci/enterococci. Furthermore, the pneumococcus typically occurs as lancet-shaped pairs, often seen in the sputa of patients with bacterial pneumonia in the presence of high numbers of polymorphonuclear (PMNs, or "polys") white blood cells; such a direct Gram stain is considered diagnostic for the pneumococcus. |
|
Staphylococci grow as large gray or white to yellow colonies on sheep blood agar. They show more robust growth under areobic than anaerobic conditions. They may be beta- or non-hemolytic. Unlike the streptococci and enterococci, staphylococci are catalase positive. Colonies of S. aureus are frequently yellow (color enhanced on chocolate agar) and beta-hemolytic. Coagulase-negative staphylococci (CNS) colonies are frequently gray to white and non-hemolytic. A trained microbiologist usually can discriminate S. aureus from CNS by colony morphology alone prior to performing any testing, but to prove the identification a coagulation test (slide coagulation and/or tube coagulation, depending upon the specimen source) is performed. S. aureus is coagulase-positive; CNS is coagulase-negative, within generally acceptable limits. If CNS is recovered from the urine of a female, susceptibility testing against novobiocin may be performed. Novobiocin-sensitivity excludes the possbility of the isolate being S. saprophyticus, while resistance to novobiocin is consistent with an identification of S. saprophyticus. As with Group A Streptococcus pyogenes (see below), Staphylococcus aureus is a very virulent organism (even though it can be found as normal skin flora), and in most cases when it is speciated it should be reported along with susceptibility test results. |
|
Streptococci grow as small gray colonies on sheep blood agar, where they may exhibit alpha- or beta-hemolysis, or they may be non-hemolytic. In contrast to the staphylococci, the streptococci show more robust growth under anaerobic than aerobic conditions and are catalase negative (the enterococci are catalase negative or weakly positive). The streptococci share many characteristics with the enterococci including the catalase reaction, but a trained microbiologist usually has little trouble distinguishing between the phenotypic characteristics of the two genera. The first step in identifying streptococci is to make careful observation of growth characteristics on sheep blood agar:
Gray alpha-hemolytic colonies may be suspected of being S. pneumoniae, viridans streptococci, or Enterococcus sp. Of these three taxa, only the enterococci will produce a positive PYR test (red color produced after addition on N,N methyl aminocynnamaldehyde reagent after exposure to L-pyrrolidonyl-beta-naphthylamide (PYR) substrate); both S. pneumoniae and the viridans streptococci are PYR-negative. The most rapid test to discriminate between S. pneumoniae and viridans streptococci is bile solubility, in which a single drop of 40% sodium desoxycholate (a bile salt) is dropped onto a single, well-isolated colony of the alpha-hemolytic organism. After about 15 minutes the plate is re-examined. The autolytic system of S. pneumoniae is activated by the bile salt and the colony will have dissolved, whereas the viridans streptococci are bile-insoluble, and the colony will remain intact on the plate. An alpha-hemolytic colony whose morphology resembles that of Enterococcus more than it resembles the viridans streptococci or the pneumococcus but which is PYR negative may be a Group D Streptococcus. Alpha-hemolytic Group D streptococci are sometimes encountered as significant pathogens urine cultures, although they may also (rarely) cause endocarditis and/or septicemia. Like the enterococci, Group D streptococci are able to grow in the presence of 40% bile esculin and to hydrolyze esculin, while other streptococci are not, and can be identified by these tests. The viridans streptococci are generally of low virulence, although they are found in about 50% of cases of subacute bacterial endocarditis, particularly in immunocompromised patients after a transient bacteremic event such as orthodontal manipulation. Some microbiologists consider the non-hemolytic streptococci to be part of the viridans group, although "viridans" refers to the greening of blood agar. Non-hemolytic streptococci are usually found as non-pathogenic contaminants or as part of a mixed culture, including after a transient bacteremic event such as orthodontal manipulation. The finding of an apparent non-hemolytic streptococcus should prompt the microbiologist to exclude enterococci (which are PYR positive), Group D streptococci (which grow in the presence of 40% bile and which hydrolyze esculin), weakly-hemolytic group B S. agalactiae (consider especially colony morphology, specimen type, numbers of organism present, and perhaps a specific test such as latex agglutination for Group B S. agalactiae), and L. monocytogenes (colony morphology nearly identical to that of Group B S. agalactiae, but a catalase-positive Gram-positive rod). To some extent the approach to identifying beta-hemolytic streptococci depends upon the specimen type. Group A S. pyogenes is the most important streptococcal human pathogen. It produces a small to medium gray colony with a small zone of beta-hemolysis and is most commonly recovered from a throat culture, where it produces pharyngitis and tonsillitis most frequently in children aged 5-15 years. Asymptomatic carriers in the upper respiratory tract and on the skin are often responsible for the spread of infection. It is important to diagnose and treat "strep throat" not so much because of the pharyngitis per se but because of the possible sequelae including rheumatic fever and acute glomerulonephritis. Although other streptococci may be associated with pharyngitis they are not associated with these sequelae, and antibiotic treatment is therefore not indicated in the absence of a positive finding of Group A S. pyogenes, since the possibility of the emergence of antimicrobial resistance outweighs any therapeutic benefit. Group A S. pyogenes recovered from any other site such as wound, fluid, or blood cultures should be considered to be a serious pathogenic threat since the organism can be highly virulent and rapidly lethal. (Occasionally Group A S. pyogenes is found in low numbers in urine cultures, especially in the presence of mixed flora, when it is probably present as normal flora, although mention of its presence even in low numbers may be indicated.) Group B S. agalactiae produces a medium gray colony with a small to very small zone of weak beta-hemolysis which sometimes may be observed to occur only directly underneath the colony after the colony has been physically removed from the blood agar plate. The colony thins gradually at the periphery producing a typical "hazy beta" colonial morphology. This organism is recovered especially from female urogenital sites (including, not uncommonly, urine cultures), from newborn blood cultures, and occasionally from wound cultures. About a third of women are asymptomatic vaginal carriers of Group B S. agalactiae, but the organism can cause severe neonatal infection including pneumonia, meningitis, and septicemia of the newborn. Wound infections with Group B S. agalactiae are sometimes encountered, sometimes in diabetic patients. On the basis of colony morphology alone, Group B S. agalactiae can be confused with the catalase-positive, Gram positive bacillus Listeria monocytogenes. Non-Group A, non-Group B beta-hemolytic steptococci produce small to medium gray colonies with large zones of strong beta-hemolysis and are recovered especially from oropharyngeal cultures, where they are rarely confused with S. pyogenes. They are of minimal virulence. |
|
Enterococci grow as small to medium gray colonies on sheep blood agar. Like the streptococci, they show more robust growth under anaerobic than aerobic conditions. They may be alpha-, beta-, or non-hemolytic. They are catalase negative or weakly positive, unlike the staphylococci, which are vigorously catalase positive. A weakly positive catalase reaction may be as little as a tiny stream of bubbles after a short delay of time. The enterococci have always been dogged by controversy in medical microbiology, and they have become even more controversial recently since (1) they were taxonomically separated from the streptococci when the genus Enterococcus was created in 1984, and (2) they first demonstrated resistance to vancomycin in 1986. Before 1984 the enterococci still were in the genus Streptococcus, although it had long been appreciated that their ecology differed significantly from that of other streptococci; specifically, enterococci are found as normal flora in the large bowel, while the streptococci are found more commonly as oropharyngeal organisms. Indeed, in many respects the enterococci are best thought of as being similar in ecological aspects to the enteric Gram-negative rods, although the enterococci just happen to be Gram-positive cocci. Still, from a clinical microbiologist's perspective, they appear similar to streptococci in both Gram stain and colonial morphology. They are catalase-negative or (more commonly) weakly positive, and they can be alpha-, beta- or non-hemolytic on sheep blood agar (by far most human isolates are weakly alpha-hemolytic or non-hemolytic, and beta-hemolytic enterococci are very rarely encountered). Also, like Group D Streptococcus spp., the enterococci can grow in the presence of 40% bile salts and hydrolyze esculin, and they express the Lancefield Group D antigen; unlike Group D Streptococcus spp. the enterococci are PYR-positive. For these reasons the enterococci are identified using the same protocol as the streptococci in the clinical microbiology laboratory, but it should never be forgotten that ecologically their behavior is much closer to enteric Gram-negative rods than it is to the streptococci. |