Diseases
of Nasopharynx
- Neoplastic
Benign: -
Nasopharyngeal angiofibroma.
Hemangioma.
Malignant:
Squamous cell carcinoma most common.
Lymphoma.
Nasopharyngeal angiofibroma:-
Commonest benign tumour (rare)
Pathology:-
Arises from lateral wall of nasopharynx
Spread:
Anteriorly: nose,
orbit, ethmoid
Inferiorly: oropharynx
Superiorly: base
of the skull.
Gross: tougth rubbery tumour with
degree of vascularity.
Histology: vascular space with no
contractile elements, surrounded by fibrous tissues.
Incidence: virtually all males.
Age: at puberty but could vary.
Clinically:-
Symptoms:
· Nasal obstruction.
· Nose bleed.
· Otitis media with effusion.
Signs: Mass which is smooth, lobulated
and hard.
Investigations:-
Lateral view plain X-ray: mass in
the nasopharynx, should be differentiated from adenoid and antrochoanal polyps.
Angiography: would show vascular
picture.
CT scan: shows the extent of the
diseases.
MRI scan: Best with Gadolenium enhancement.
Biopsy is risky.
Treatment:-
Major task
Embolization: to reduce the vascularity
preoperatively.
Surgery: treatment of choice cross
match for several untis of blood.
Transpalatal
approach
Transantral
approach
Craniofacial
approach
How staging helps the treatment:
Stage I: Tumour limited to nasopharynx
Stage II (A) Tumour spread to ethonoid,
sphenoidsinus.
(B)
Lateral spread to pterego palates fossa, infra temporal fossa,
cheek.
Stage III Superior
and lateral spread.
Stage IV Intra
cranial extension craniotomy.
Nasopharyngeal carcinoma:-
Commonest tumour of the nasopharynx, common in Chinese race
accounting for up to 18% of all malignancy in China.
Aetiology multifactorial:
1.
Genetically determined susceptibility HLA A2.
2.
EB virus (Epstein-Berr Virus) infectious in early life.
3.
The integration of the genomes of the virus into chromosomes
in the nasopharynx.
4.
Some environmental neoplastic transformations that gain entry
into infected cells. (Salt fish ingestion in China.) Nitrosamine.
Incidence:
male: female = 2:1
Age: 5th decade.
Clinically:
30% nasal symptoms: obstruction, bleed.
20% deafness
20% Neck gland (metastasis)
10% pain
20% cranial nerve palsy IX, X, XI,
XII
Check for push of the soft palate
downwards, fluid in the ears, paralysis of the tongue, III, IV, VI eye movement, trismus and facial numbness.
Neck examinations distant spread to
lungs, liver and bones.
Investgations:
1.
EBV sorology for high risk patient and IgA antibody for the
VCA (viral capside Antigens)
2.
Radiography:-
Plain X-ray: destruction of base of
skull 30% and chest X-ray indicated.
CT scan: showed soft tissue involvement
into retropharyngeal and pharapharyngeal spaces, and also intracranial extension.
MRI scan: Best to detect intracranial
extension.
3.
Biopsy: from fossa of Rosenmuller
Classification of SCC of nasopharynx:
Based on light microscopy
5 year survival.
Type I: 25% of NPC, well differentiated (keratinised)
10%
Type II: 12% of NPC, variable differentiation
(minimal keratinsation) 50%
Type III: 60% NPC, undifferentiated
(Anaplastic).
60%
TNM classification
TX: primary tumour cannot be assessed.
T0: No evidence of primary tumour.
Tis:
Carcinoma in situ.
T1: tumour confined to nasopharynx.
T2: Tumour extends to soft tissue.
T2a: tumour extends to oropharynx
and or nasal cavity without parapharyngeal extension.
T2b: any tumour
with parapharyngeal extension.
T3: Tumour invades body structure/
paranasal sinuses.
T4: Tumour with intra cranial extension,
cranial nerve involvement, infratemporal fossa, orbital involvement.
Treatment:-
Radiotherapy in the treatment of choice,
neck should be included: dose 6500-7000 cGy.
Complication of radiotherapy:
- Xerostomia.
- Tooth
decay.
- Hypopituitism,
hypothyroidsim.
- Eye
problems.
- Skin
problems.
- Skull
bone necrosis.
- Osteoradio
necrosis for the bone.
Surgery: for neck glands (radical
neck dissections).
Biopsy nasopharynx for diagnosis.
Chemotherapy: mainly for palliative
management.
Immune therapy: including vaccines
in the future.
Prognosis:-
Depends on the stage of the tumour
(15% - 75%)
Other pharyngeal tissues:-
- Lymphoma.
- Salivary
gland tumour.
- Carcomas.
Adenoids:
Definition: hypertrophy of nasopharyngeal tonsil sufficient
to produce symptoms (arises from the roof and posterior wall of nasopharynx. (ages 3-10).
What is the difference between palative tonsil and adenoids.
Pharyngeal tonsils the adenoid has:
- No
crypt.
- No
capsule.
- Ciliated
epithelium cover.
Problems with adenoid:
Symptoms of signs:
In infants:
· Failure to thrive.
With older children:
· Breathing through the mouth.
· Snoring.
· Loss of tone in voice.
· Nasal discharge cough.
· Dental malocclusion.
- Eustachion
tube obstruction:
Glue ears with
deafness.
- Others:
- Rhinitis.
- Mental
dullness.
- Nocturnal
enuresis.
- Nightmares.
Investigations:-
1.
Rigid nasoendoscopy: small telescope (2.4mm) maybe suitable
for older children.
2.
Post nasal space X-Ray not always helpful.
3.
Examination under G.A.
Treatment: -
Removal under G.A using adenoid curette
Complications:-
· Bleeding primary, reactionary and secondary.
· Recurrence
· Damage to the Eustachion tube.
· Hypernasality with nasal escape.
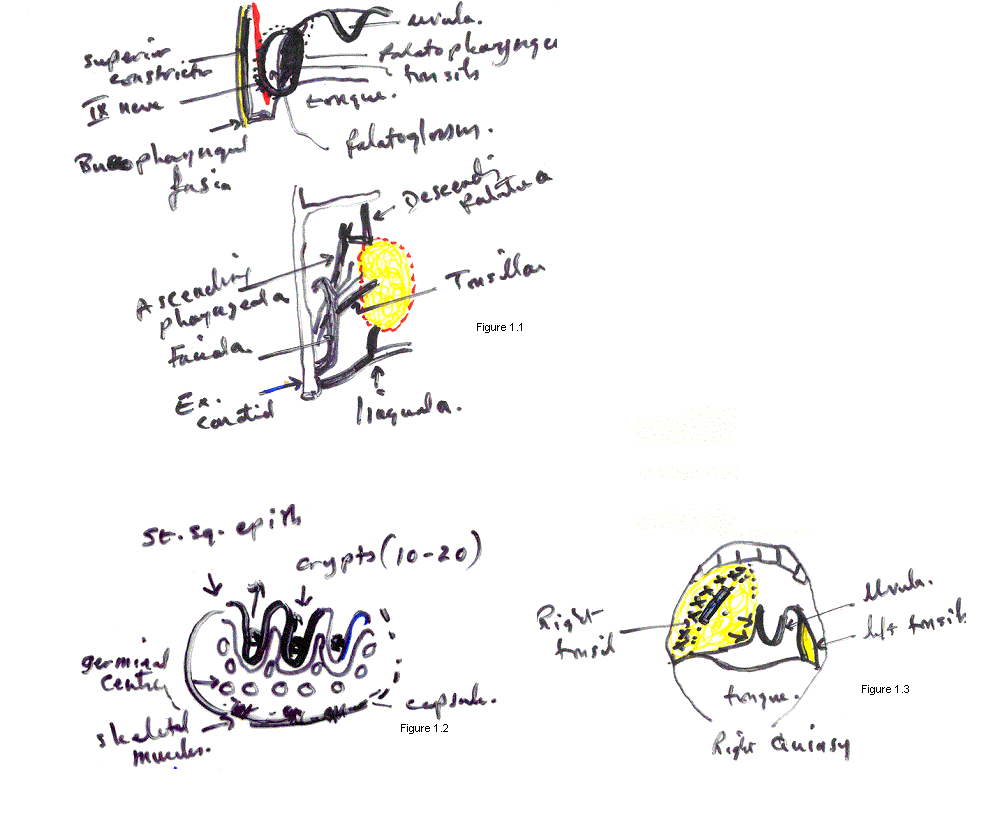
Tonsillar anatomy
and disease
Definition: lymphoid tissue in the oropharynx
Relation:
Anteriotly: palatoglossal arch
Posteriorly: palatopharyngeal arch
Medially: free surface
Laterally within outward:-
Capsule.
Superior constrictor muscle, IX nerve,
facial artery.
Buccopharyngeal fascia.
Blood Supply:-
Arteries:
Veins: forms a plexus which communicates above with pterygoid
plexus and drains into common facial and internal Jugular vein.
Nerves: IX and X
Lymphatic drainage: into upper Jugulo digastric nodes.
Structure:
Waldeyer's ring: (lymphoid tissue in the head and neck)
- Lingual
tonsils.
- Posterior
pharyngeal wall lymphoid tissue.
- Lymphoid
tissues in the fossa of Rosenmuller.
- Nasopharyngeal
tonsil.
- Palatine
tonsils.
Function:-
Group of secondary lymphatic organs which represent 0.2% of
all lymphocytes in adult. It ceases to function after birth and the studies show that removing chronically inflamed tonsils
would increase the IgA in the body which enhances the immune system.
Tonsillar diseases:-
Tonsillitis:
- Acute:
· Aetiology:
Haemolytic streptococci.
Viral infection.
Others: staphylococci, Haemophilas
influenza.
· Symptoms:
Sudden onset
Temperature rises up to 40°C.
Considerable swallowing
problems.
Earache.
Abdominal pains
due to mesenteric lymphadenitis
· Signs:
Enlarged red and swollen tonsils with
crypt full of Fibrin turns into purulent and necrotic areas.
Enlarged cervical
glands.
Increased pulse
rate due to fever.
· Investigations:
Throat swobs. (controversal)
FBC
Mosospot test.
· Treatment:
Bed rest.
Pain killer: paracetomol
with codein.
Non steriodal anti-inflammatory.
(like voltarol)
Antibiotics: penicillin
is the treatment of choice.
Avoid ampicillin
as it causes rash.
Fluids.
· Complications:
Peritonsillar absess.
Parapharyngeal
and retropharyngeal absess.
Septicaemia.
Others: larygeneal
oedema, nephritis, chronic tonsillitis.
- Chronic
tonsillitis:
Recurrent short-lived bouts of febride
malaise with sore throat, red tonsils.
Indication for tonsillectomy:
1.
Recurrent tonsillitis at least 4-5 episodes per year in the
past 3 years.
2.
Peritonsillar absess after 2nd episode.
3.
Unilateral tonsillar enlargement.
4.
Gross tonsil enlargement à obstructive sleep apnea.
- Peritonsillar
absess (Quinsy):-
Definition:
Suppuration (absess)
outside the tonsillar capsule.
Incidence:
More unilateral
and mainly in adults.
Symptoms:
Increased temperature
with rigor 40°C.
The patient looks
ill.
Acute sore throat.
Ear ache, Foeter
oris (bad breath).
Inability to swallow
Signs:
Trismus
Oedema of the uvula
which is pushed to the other sides of the infection.
Enlarged cervical
glands.
Treatment:
Drainage under
L.A using scalpel or aspiration using 10ml syringe.
I.V antibiotics:
penicillin is the choice.
Complications:
Parapharyngeal
absess.
Haemorrhage.
Laryngeal obstruction,
air way obstruction.
- Tonsillar
tumour incuding oropharyngeal
Classification:
Benign adinoma, papilloma.
Malignant squameous cell carcinoma 75%.
Lymphoma 15%
Minor salivary glands 5%
Incidence:
M : F = 10 : 1
Etiology:
Smoking and alcohol.
Clinical features:
Symptoms:
Sore throat.
Otalgia.
Disphagia.
Tonsillar bleeding.
Signs:
Squaemous cell carcinoma always ulcerated.
Lymphoma causes unilateral enlargement of the tonsils.
Investigations:
Haemotological H.P for anaemia.
Radiological chest X-Ray
OPT for bone involvement.
CT scan to check tumour extent.
Classifications:
UICC:
T1 tumour less
than 2cm
T2 2-4 cm.
T3 more than 4cm.
Treatment:
Depends on the staging and the fitness of the patient.
In general surgery is highly indicated except for very small tumour where
radiotherapy is indicated.
Surgery:
Commando procedure involves the removal
of part of the soft palate, part of the tongue, part of the mandible with radical neck dissection and cover the defect with
free flap (radial forearm flap).